Sleep-Disordered Breathing (SDB)
Sleep-Disordered Breathing (SDB) is a cause of poor quality sleep and can lead to long term fatigue and health problems if not diagnosed and treated. What are the different forms of SDB and how can you distinguish them?
What is SDB (Sleep-Disordered Breathing)?
SDB (Sleep-disordered Breathing) covers both UARS (Upper Airway Resistance Syndrome) and OSA (sleep apnea). Both conditions are concerned with the passage of air (oxygen) into the lungs, but they manifest with different symptoms and have different profiles and treatments.
Some people find it difficult to breathe through their nose during sleep. Problems with the nasal passages are known as UARS (Upper Airway Respiratory Syndrome). This condition is caused by congestion in the tissues of the nose itself, which is often brought about by yeast overgrowth (Candida). Snoring is often part of the syndrome.
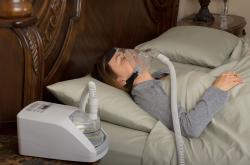
The other type of SDB – sleep apnea - is when the throat collapses during sleep. This leads to lack of oxygen and waking (or semi waking) with a gasping sound. Despite the fact that the blockage of air is more severe in sleep apnea, the actual symptoms of UARS can be more acute. In fact, they can often mimic the symptoms of CFS (chronic fatigue syndrome) and fibromyalgia.
The treatment for UARS is different from that for sleep apnea, so it’s really important to distinguish between them. Both conditions cause fatigue and tiredness. UARS tends to cause more exhaustion during the day because of the extra effort to breathe during the night.
What is the difference between UARS and sleep apnea?
Chronic insomnia, with a pattern of constant awakenings and failure to fall back into sleep is more common in patients with UARS than sleep apnea is. UARS affects the sexes equally (about 50% women and 50% men) while sleep apnea (OSA) tends to be more a problem that men have (over 90% of sufferers are male). People with sleep apnea are likely to be overweight but those with UARS can be any weight.
Patients with OSA tend to fall asleep easily during the day. They have an increased risk of automobile accidents (estimated at between two and eightfold increased risk). Those with UARS on the other hand tend feel fatigued but not to feel sleepy or to fall asleep.
There are quite different patterns to blood pressure as well. Patients with sleep apnea tend to be hypertensive (to have high blood pressure) while those with UARS generally have low blood pressure and light headedness on standing.
Interestingly, UARS often presents with a spastic colon as well as cold hands and feet. The latter two symptoms are often part of the picture of clinical hypothyroidism (when the thyroid gland doesn’t produce enough hormones).
UARS has a symptom in common with CFS (chronic fatigue syndrome) and fibromyalgia: a brain-wave pattern called alpha intrusion into delta sleep. This makes deep sleep shallower, as deep sleep is normally composed only of delta and theta brain waves and alpha brain waves belong to lighter sleep.
Actually, there is a considerable overlap between sleep-disordered breathing, CFS and fibromyalgia. Many people suffer from both. There is a gender difference, however. In a study of those with sleep-disordered breathing 50% of women, but only 6% of men were found to have fibromyalgia.
How can UARS and sleep apnea be diagnosed?
Both disorders probably need a good sleep lab to be diagnosed successfully. UARS now can be detected with recently introduced technology, which monitors pressure changes in your nose or alterations in your breathing patterns.
There is a simple test that you can do if you are unable to go to a sleep lab that specializes in UARS. Looking at you face in a mirror, press the nostril on one side of your nose in order to close it. Now close your mouth and breathe through the other nostril. If the nostril tends to collapse, try holding open with the flat side of a toothpick. If breathing is easier with one nostril held open in this way, try using nasal dilators or nasal strips when sleeping.
Sleep apnea is diagnosed with a battery of sleep lab tests, including an overnight EEG (electroencephalogram), which measures the brain-wave patterns during sleep. Sleep apnea disturbs deeper sleep, so this should be apparent on the machine’s print-out. Respiratory monitors can both measure airflow and detect if the oxygen in the blood is dropping and by how much.
If you videotape yourself at night and watch the tape later, you will probably be able to detect the differences between sleep apnea and UARS. Sufferers from sleep apnea will tend to stop breathing and then take in air with a sudden gasp, whereas those with UARS will be quieter.
There is a fair amount of debate about how common sleep-disordered breathing is. Unfortunately, most physicians receive very little training in sleep disorders. This is perhaps because mainstream medicine has not yet recognized the effect of high quality sleep on health generally. Estimates of the prevalence of sleep apnea vary between 3% and 17% of the general population. Such a wide variation suggests that many medical practitioners are not especially aware of the condition. This is borne out by studies which have shown that, once doctors received specific training about sleep apnea, the number of patients they sent for sleep testing increased dramatically.
[Please seeUARSandSleep Apneafor more information on both of these conditions].





.jpg)







Leave a comment